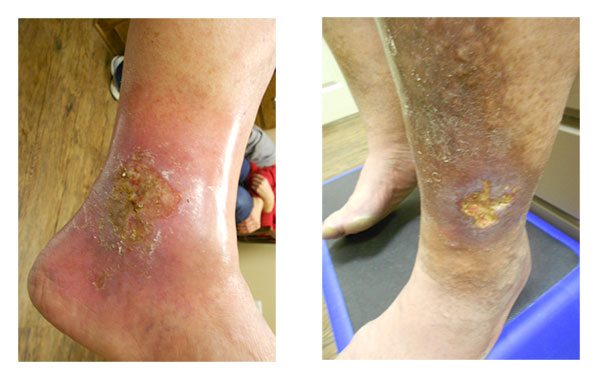
Leg ulcers, also known as venous ulcers, can often be perplexing for both patients and many physicians who lack expertise in vascular surgery. In this article, our mission is to provide clear answers regarding leg ulcers. Let’s start by delving into the root causes of leg ulcers.
What are leg ulcers?
Leg ulcers (venous ulcers) can be as confusing to patients as they are to many physicians, who don’t have experience in wound care, and who aren’t vascular surgeons. These wounds appear in the lower leg are the subject of all kinds of speculation by non surgeons, including what causes leg ulcers, why they return, and how they can be treated. In this article, we hope to provide the solid answers for those of you dealing with these sores. Let’s begin with what actually causes them.
What causes venous stasis ulcers?
The problem begins with poor circulation in the legs. The circulation problem could involve arteries, veins or both. Patients who smoke, have diabetes, peripheral obesity or poor nutrition are at especially high risk for having arterial disease. Patients with long standing bulging, varicose veins and leg swelling are at risk for developing venous disease, particularly if they have developed the thickened and discolored skin associated with long stand vein disease.
Venous stasis ulcers do not occur in all patients with varicose veins, and may occur in the absence of varicose veins. We cannot definitively predict who will go on to develop this complication. When skin changes begin to appear, the likelihood of ulceration increases. It is obviously better to treat the vein problems before this occurs.
Although many physicians who aren’t experienced with the treatment of leg ulcers believe that they occur spontaneously, it is more likely that they occur following what would be an insignificant trauma, because the skin is already compromised, and fail to heal because of unfavorable circulation.
Are leg venous ulcers dangerous?
Yes, if they are not diagnosed appropriately. Although venous stasis ulcers are rarely limb threatening, if an arterial issue is mistaken for a vein issue, and the arterial issue is not properly addressed, you could end up with an amputation. Not all specialists treating veins are vascular surgeons. There are specialists, such as radiologist, who have little experience in patient care, and who believe that treatment of veins begins and ends with putting a catheter in a vein and using heat to close it. They don’t realize how much they don’t know, and often have difficulty in differentiating between arterial and venous disease.
Evaluation before treatment is important
Arterial circulation must be assessed prior to embarking on treating venous disease. A vascular surgeon can determine whether your arterial circulation is adequate, prior to performing any venous procedures. The surgeon treating your veins needs to also understand the principals of treating wounds, and be able to manage not only the circulation issues, but also the wound.
How do I treat venous leg ulcers?
Once the arterial circulation has been assessed, the venous stasis ulcer can be addressed. When reflux is left untreated over many years, the constant pressure may cause a leaking of inflammatory cells into the tissues. This causes brown staining of the skin is known as venous stasis changes and indicates that the venous insufficiency has become more severe.
If this process continues, a breakdown of the tissue may occur resulting in a venous stasis ulceration. Venous stasis ulcers are painful, and are chronic in nature with the ulcer reopening just when it appeared to be healed.
There are two components to treatment:
- The first is addressing the wound care for the ulcer. The most common treatments of venous leg ulcers are compression dressings impregnated with medication, which also aid healing, reduce edema (swelling) and prevent inflammation. These dressings are referred to as unna boots.
- The second issue regarding treatment of venous stasis ulcers is addressing the cause. If venous insufficiency is present it should be addressed. Treatment of the venous insufficiency will usually facilitate healing and reduce the incidence of recurrence.
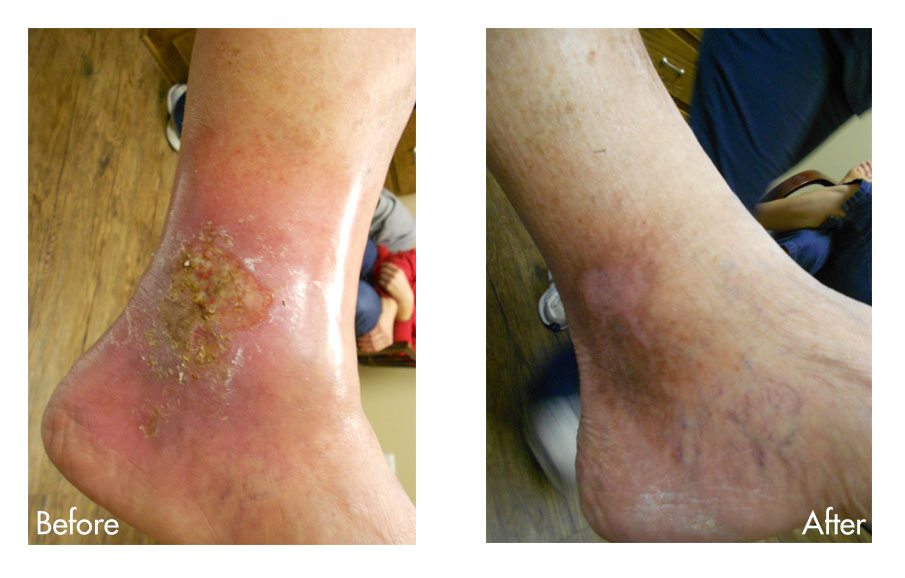
Venous Stasis Ulcers – Before & After Photos
Venous Ulcers Treatments in Houston
Get your veins treated by a top vein specialist in Houston, Dr. Bardwil. Call Texas Vein & Cosmetic Specialists today to schedule your initial evaluation. You can find us in our two locations: Houston, our main location, or Katy.
Dr. Bardwil has meticulously written or reviewed all the website content, ensuring that all the medical facts in the text are correct.